In our highly medicated society, Americans consume more mind and mood altering drugs—legal, illegal and prescribed–than any other people in the world. Cocaine, heroin, marijuana, Xanax, Ambien, Atavan, alcohol and many more: a full spectrum of pain, anti-anxiety, anti-depressant and stimulating medications.
We all know people affected by the overuse of these substances. Some of us know people who have died from them.
But why are we in so much pain? So depressed? Why can’t we sleep? Or focus?
Structural pain
Sometimes the cause is clear: You are hit by a car or fall off a ladder.
Or it may be more subtle–slow and steady—caused by long days spent staring at a computer screen, delivering kegs of beer or flipping mattresses.
In each of these cases, ligaments and muscles are torn, joints are swollen and nerves are irritated. And we feel pain.
Psychic pain
But there is another kind of pain that begins at a deeper level; one that can’t be reduced to inflamed soft tissue. It’s a pain that arises from the interplay of mind and body, of our emotions, our chemistry and our structure.
The post-traumatic stress of a violent encounter, the break up of a relationship or the low grade despair of a life lived without meaning can effect all of the systems of our body. Changes in blood and hormone flow, muscle tension and heart rate may cause sleeplessness, anxiety, distraction, depression or chronic pain.
Whether a blowtorch-wielding steel worker or a corporate lawyer, no one is immune to the impacts of physical or emotional stress. The pressures of modern living are increasing steadily. The 50-hour workweek has replaced the 40, and for many it is more than that. Economic insecurity keeps many people from even taking their allotted vacation time. Fear of being replaced drives people to work themselves into exhaustion.
Treatment: two approaches
People come to see me when they are in pain. I examine, diagnose and treat. I loosen their muscles and manipulate their joints. I prescribe exercises and explain appropriate work behavior. I ask about life style. How are they managing their stress? Are they breathing properly? Eating well? Taking time just for themselves? Then I recommend strategies designed to heal, and to prevent acute problems from becoming chronic.
That same person may find himself in a medical office that takes a very different approach. “Having back pain? Here is a prescription for an anti-inflammatory (e.g. Naproxen), a muscle relaxer (e.g., Robaxin) and a painkiller (e.g. Vicodin). The back pain is chronic? Try this anti-depressant (e.g. Elavil). Anxiety? Atavan. Can’t sleep because of the pain or anxiety? Ambien will help with that.”
And though some patients may see their problems resolve with this regimen, many others end up using these medications chronically. Without addressing causes, the underlying problems can persist—fueling the desire/need for ongoing and increasing dosages.
The deadly “cures”
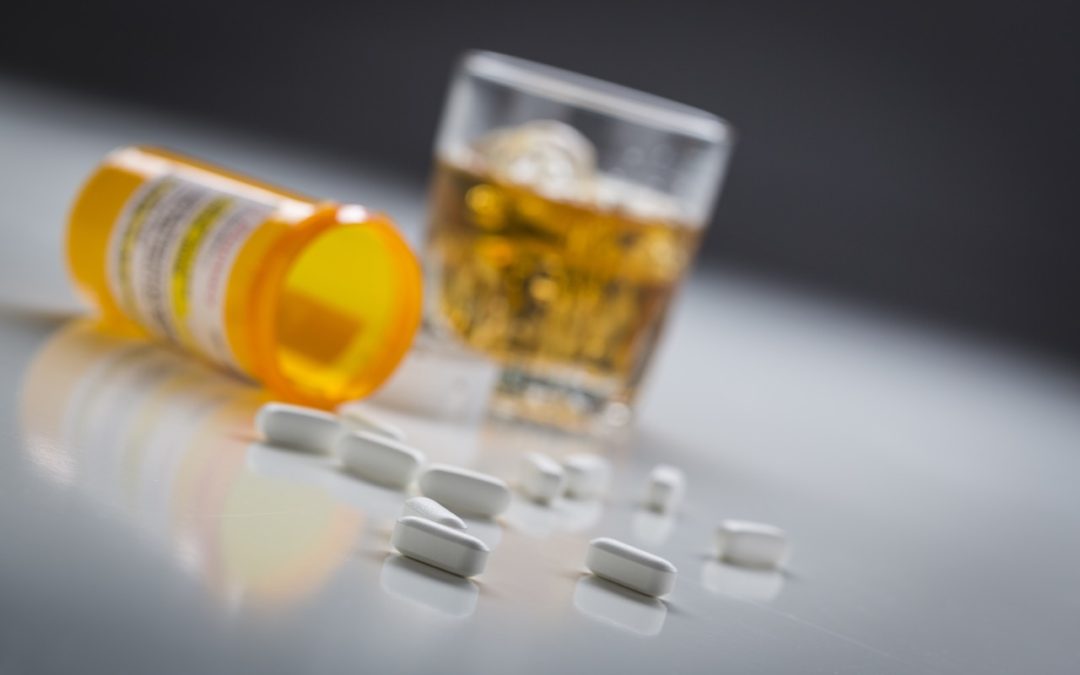
When pain becomes chronic, the physical and psychic merge and patients may start combining medications. A fentanyl patch for the hip pain that started with a fall at work, a Xanax for the anxiety of being on disability due to the work injury, an Ambien to help get to sleep and perhaps a shot or two of Jack Daniels to “relax” before bed.
This pharmaceutical strategy can escalate into full blown addiction. Let’s say a medical doctor limits the prescription of oxycontin because she suspects a patient is abusing his medication. This might send that patient into the street to buy the much cheaper (and easily acquired) black tar heroin which also does the trick.
We all know the sad ending to these stories. The actor Heath Ledger, the great rock star Prince, and Deb, the piano player in one of my bands. Thousands of young people from big and small towns around the country. All dead. And the toll is mounting.
The Hippocratic Oath
The modern version of the Hippocratic Oath–the vow taken by physicians upon graduation from their professional schools and prior to embarking on their careers–contains several statements worth noting:
“I will prevent disease wherever I can, for prevention is preferable to cure.”
“I will apply, for the benefit of the sick, all measures which are required, avoiding the twin traps of over treatment and therapeutic nihilism.”
“I will not be ashamed to say ‘I know not,’ nor will I fail to call in my colleagues when the skills of another are needed for a patient’s recovery.”
Too often, those in the healing professions violate these principles. Economic realities embedded in a competitive marketplace, fueled by a perception of scarcity, can push providers to favor collections over care.
At the same time, Big Pharma pumps out medications for every ailment. The more chronic, the better; meds for a lifetime are best. There is no money in prevention. Ongoing prescription means easy, steady office visits.
And my profession is no different. Prescribing endless treatments using questionable X-ray diagnostics, chiropractors can foster patient dependence. Few would admit, however, that these are business practices aimed at maximizing profits.
Finally, both traditional MD’s and alternative practitioners can allow their egos to inhibit referrals to providers outside of their professions. In most medical schools there are few (if any) classes that focus on specialties outside the traditional medical world. MD’s know all about neurologists, nephrologists, gastroenterologists and all the other “ists,” but very little about chiropractors, acupuncturists, naturopaths or pilates instructors. And alternative providers can be grandiose in their appraisal of what conditions they can effectively treat. How can a practitioner refer a patient to seek help beyond one’s own narrow scope, when one sees nothing outside it?
A better approach
The pain we all feel is real. The causes can be clear or subtle. But we must ask ourselves whether we want to treat only the symptoms, or to determine the causes and make corrections there.
This approach may frighten both patients and providers, forcing the former to take responsibility for their health and the latter to leave economics out of their health care recommendations. It compels all of us to look at the world we have constructed, and consider challenging the notion that the reality we know is the only one there is. Only then can we get to the root of our pain.
Dr. Ricky Fishman has been a San Francisco based chiropractor since 1986. In addition to the treatment of back pain and other musculoskeletal injuries, he works as a consultant in the field of health and wellness with companies dedicated to re-visioning health care for the 21st century.
ricky@rickyfishman.com www.rickyfishman.com











As usual, a thoughtful, articulate piece, Dr. Ricky. In my own work (as a psychotherapist), there are instances when it is quite clear the ‘problem’ or what ails is the very social and cultural gestalt (or shall we say, ‘matrix’) within which a patient’s or client’s existence is embedded and rationalized as that’s all there is … as in the Peggy Lee song, “Is That All There Is?” (1969, https://www.youtube.com/watch?v=WNFe4nak-oM). ‘All there is,’ in the context of your blog piece, refers to that 50-hour gotta-get-ahead work week, that body-wrecking multi-hour mired-in-stasis position in front of computer screens, that el quicko MacShit & Starbugs lunch on the run, that steady diet of televised canned news and mass distraction entertainment, & so on. I suppose ‘treatment’ at times might well begin with keeping still long enough to allow for visions or experiences of alternative possibilities outside of the Matrix to emerge. Your closing sentence sez it all: “[Such an approach] … compels all of us to look at the world we have constructed, and consider challenging the notion that the reality we know is the only one there is. Only then can we get to the root of our pain.”
Ben thank you so much for your thoughtful comment. Just as mind and body are one, so are we and the world in which we live.The “illness” or the pains we suffer cannot always be isolated (reduced) in the body but rather are “located” in the space in which our mind/bodies connect to the world.